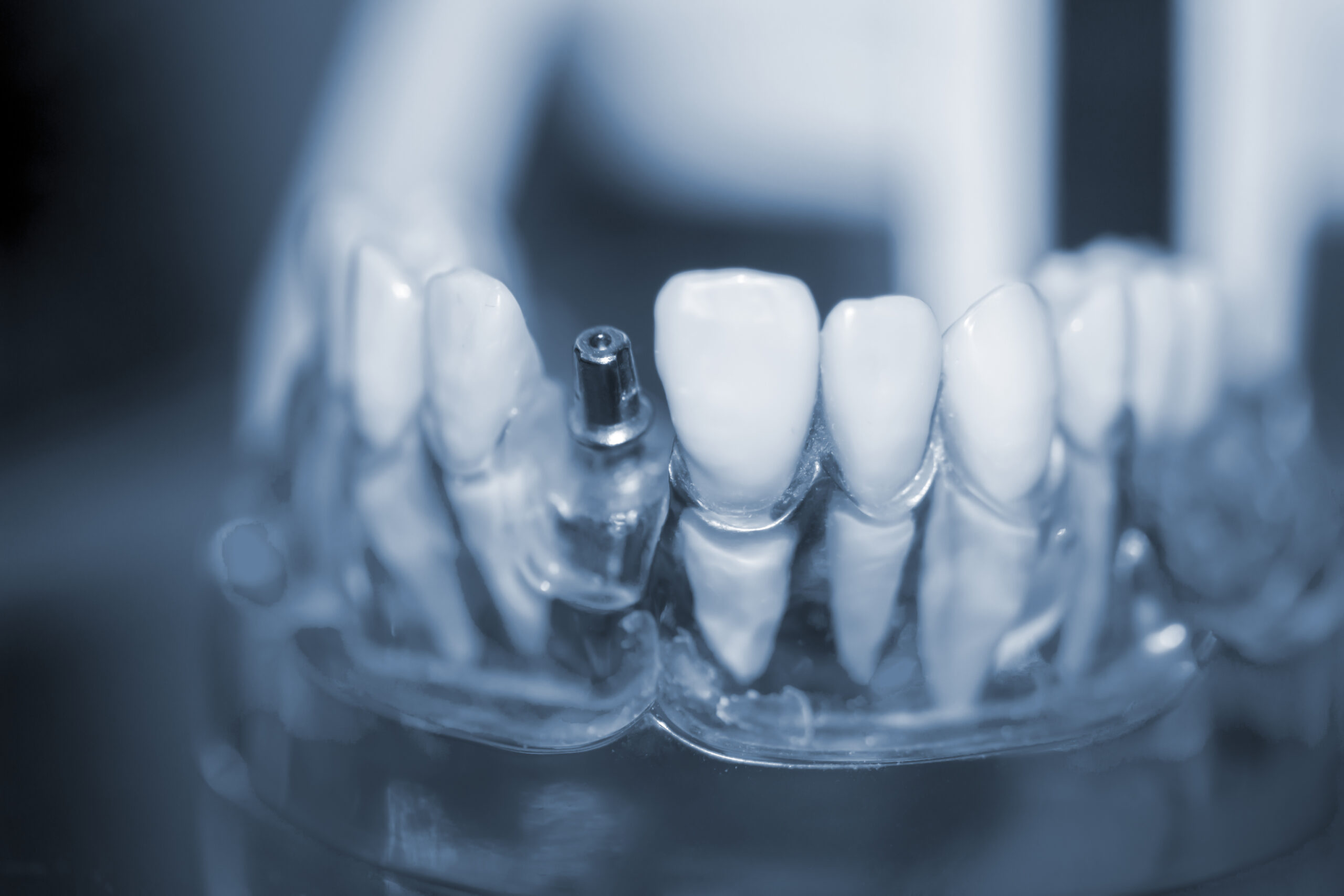
From a medical perspective, dental implants are not “rejected” by the body.
The body does not react with an active rejection response.
What can happen instead usually has other causes:
Either the implant does not properly bond with the bone during the healing phase (this is called failed osseointegration), or an التهاب develops in the tissue surrounding the implant (known as peri-implantitis).
Neither of these situations means that the body is actively “rejecting” the implant.
What actually happens in your body
After an implant is placed, something crucial begins:
Your body works to firmly integrate the implant into the jawbone. This process is often described as the implant “healing in” or “fusing” with the bone. Step by step, the bone grows onto the implant surface and anchors it securely in the jaw.
This process is called osseointegration.
If it is successful, the implant becomes a stable part of your jaw—allowing you to chew normally, almost like with a natural tooth.
What if the implant does not heal properly?
This is the situation many people describe as “rejection.”
In reality, the implant has simply failed to bond sufficiently with the bone. As a result, it may remain slightly mobile or gradually lose stability over time.
Common reasons include:
- Insufficient initial stability in the bone
- Excessive stress or irritation during placement
- Reduced blood supply in the area
- Conditions such as diabetes affecting healing
- Smoking, which significantly impairs healing
What is peri-implantitis—and why can it cause problems?
More common than poor healing is peri-implantitis, an inflammatory disease affecting the tissue around the implant, leading to gradual bone loss.
What happens during peri-implantitis?
- Bacteria accumulate on the implant surface, forming a biofilm (similar to dental plaque)
- This can lead to a superficial gum inflammation (mucositis), which is still treatable
- If untreated, it may progress to peri-implantitis
- Bone around the implant begins to break down
- Over time, the implant loses its stability and may eventually be lost
What increases the risk of poor healing or inflammation?
Implant success rarely depends on a single factor—it’s usually a combination:
- Bacterial plaque (biofilm): the most common trigger
- Poor oral hygiene
- Smoking: reduced blood flow and slower healing
- Systemic diseases (e.g., poorly controlled diabetes)
- Medications affecting healing or bone metabolism
- Bone quality: insufficient or soft bone complicates stability
- Surgical factors: heat, pressure, and positioning during placement
- Prosthetics: difficult-to-clean restorations or cement residues
- Periodontitis: introduces harmful bacteria
- Improper or premature loading during healing
How can early implant problems be recognized?
Changes usually develop gradually—and can be detected early if you know what to look for.
Early signs (often mucositis):
- Bleeding when brushing or touching the area
- Redness or slight swelling of the gums
- Changes in tissue texture (softer or more sensitive)
- Occasional pressure sensation
At this stage, the condition is still reversible.
Signs of progression (peri-implantitis):
- Increasing pocket depths around the implant (measured by your dentist)
- Bone loss visible on X-rays
- Pus formation in advanced cases
- Loosening of the implant in later stages
Important to know:
👉 Many of these changes do not cause pain at first.
This is why follow-up care is essential.
Regular check-ups allow problems to be detected early – often long before you notice anything yourself.
What happens if an implant is lost?
In rare cases, an implant may need to be removed.
If that happens, the situation is carefully reassessed:
- What is the bone quality?
- Are there inflammatory processes present?
- Is bone augmentation necessary?
Based on this, a decision is made about whether and when a new implant can be placed.
For maximum safety: treatment and follow-up from a single source
Dental implants are not rejected by the body. What matters is stable osseointegration and inflammation-free conditions around the implant.
For long-term success, three things are essential:
experience, precise planning, and reliable follow-up care.
At Lifedent Lucerne, we guide you through every step of the process.
With structured diagnostics, clear treatment protocols, and regular monitoring, we ensure that any changes are detected early and treated effectively.
👉 This creates the best possible conditions for stable, long-lasting implants.
📞 +41 41 481 00 00
🌐 www.lifedent.ch